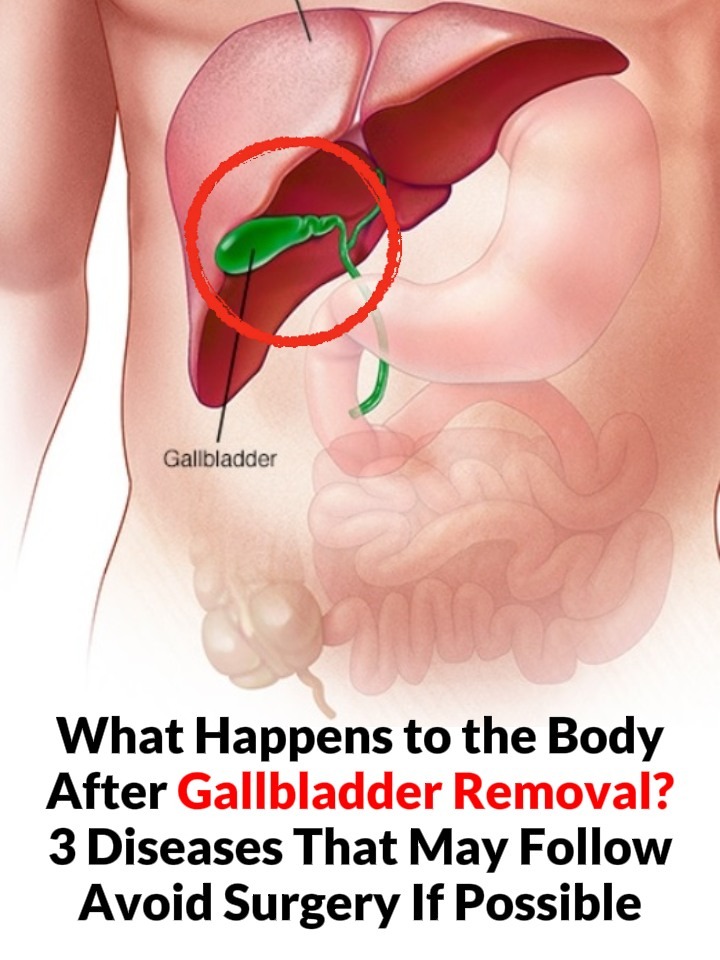
Gallbladder removal, medically known as cholecystectomy, is one of the most common surgeries performed worldwide. Doctors often recommend it for gallstones, inflammation, or gallbladder dysfunction. While the procedure can be lifesaving and necessary in many cases, it is often presented as “routine” or “harmless.”
But the gallbladder is not a useless organ. Its removal can trigger long-term changes in digestion, metabolism, and overall health. For some people, these changes are mild. For others, they can lead to chronic conditions that affect quality of life for years.
Let’s explore what really happens to the body after gallbladder removal, the three diseases that may follow, and why avoiding surgery—when medically possible—can be beneficial.
What Does the Gallbladder Actually Do?
The gallbladder is a small, pear-shaped organ located beneath the liver. Its main role is to store and concentrate bile, a digestive fluid produced by the liver.
Bile is essential for:
-
Breaking down fats
-
Absorbing fat-soluble vitamins (A, D, E, and K)
-
Supporting healthy bowel movements
-
Maintaining balanced gut bacteria
When you eat a fatty meal, the gallbladder releases a controlled amount of bile into the small intestine. This timing and concentration are crucial for proper digestion.
After gallbladder removal, this natural regulation is lost.
What Changes After Gallbladder Removal?
Once the gallbladder is gone:
-
Bile flows continuously from the liver into the intestine
-
Bile is less concentrated
-
Digestion becomes less efficient, especially for fats
-
The gut is exposed to bile even when no food is present
These changes may not cause immediate symptoms, but over time they can disrupt digestion, metabolism, and gut health.
1. Post-Cholecystectomy Syndrome (PCS)
One of the most common long-term outcomes is Post-Cholecystectomy Syndrome.
What Is It?
PCS is a collection of digestive symptoms that persist or appear after gallbladder removal.
Common Symptoms:
-
Chronic diarrhea
-
Bloating and gas
-
Abdominal pain or cramping
-
Nausea after meals
-
Fat intolerance
-
Acid reflux
Why It Happens:
Without the gallbladder, bile drips constantly into the intestines. This can irritate the intestinal lining and overwhelm the digestive system, especially when eating fatty or processed foods.
Long-Term Impact:
Some people live with PCS for years, managing symptoms with medications, restrictive diets, or repeated doctor visits.
2. Non-Alcoholic Fatty Liver Disease (NAFLD)
The gallbladder and liver work as a team. Removing the gallbladder places extra strain on the liver, which must now regulate bile flow alone.
How Gallbladder Removal Affects the Liver:
-
Continuous bile production increases liver workload
-
Fat metabolism becomes less efficient
-
Insulin resistance may increase
Over time, this can contribute to Non-Alcoholic Fatty Liver Disease, a condition where fat accumulates in liver cells.
Symptoms May Include:
-
Fatigue
-
Right-side abdominal discomfort
-
Elevated liver enzymes
-
Progression to inflammation or fibrosis in severe cases
Why This Matters:
NAFLD is now one of the leading causes of chronic liver disease. While not everyone develops it after surgery, studies show higher rates in people without a gallbladder.
3. Irritable Bowel Syndrome (IBS) and Chronic Diarrhea
Gallbladder removal significantly alters how bile interacts with the gut.
The Bile–Gut Connection:
Excess bile entering the colon can:
-
Disrupt gut bacteria
-
Increase intestinal motility
-
Irritate the bowel lining
This can trigger symptoms similar to IBS, especially the diarrhea-dominant type (IBS-D).
Common Complaints:
-
Urgent bowel movements
-
Loose stools after eating
-
Abdominal cramps
-
Food sensitivities
For some patients, this becomes a lifelong condition, requiring medication and strict dietary control.
Nutrient Deficiencies After Surgery
Because bile is crucial for fat digestion, gallbladder removal can impair the absorption of:
-
Vitamin A (vision, immunity)
-
Vitamin D (bones, immunity)
-
Vitamin E (cell protection)
-
Vitamin K (blood clotting)
Over time, deficiencies may contribute to:
-
Weak bones
-
Fatigue
-
Poor immunity
-
Skin and hair problems
Why Avoid Surgery If Possible?
This does not mean gallbladder surgery is always bad or unnecessary. In emergencies—such as severe infection, rupture, or cancer—surgery is absolutely essential.
However, many gallbladder removals are done for:
-
Mild or intermittent gallstones
-
Sludge without severe symptoms
-
Functional issues that may respond to lifestyle changes
In such cases, non-surgical approaches may be worth exploring first, under medical supervision.
Non-Surgical Options (When Medically Appropriate)
Depending on the condition and severity, doctors may recommend:
-
Dietary changes (low-fat, whole foods)
-
Weight management
-
Improved hydration
-
Medications to dissolve certain gallstones
-
Managing insulin resistance
-
Supporting liver and bile flow
Early intervention can sometimes prevent progression to surgery.
Life After Gallbladder Removal: Can People Live Normally?
Yes—many people live full lives without a gallbladder. However, “normal” often requires:
-
Long-term dietary awareness
-
Avoiding fatty and fried foods
-
Managing digestion carefully
-
Monitoring liver and gut health
Understanding potential risks allows people to prepare, adapt, and protect their health.