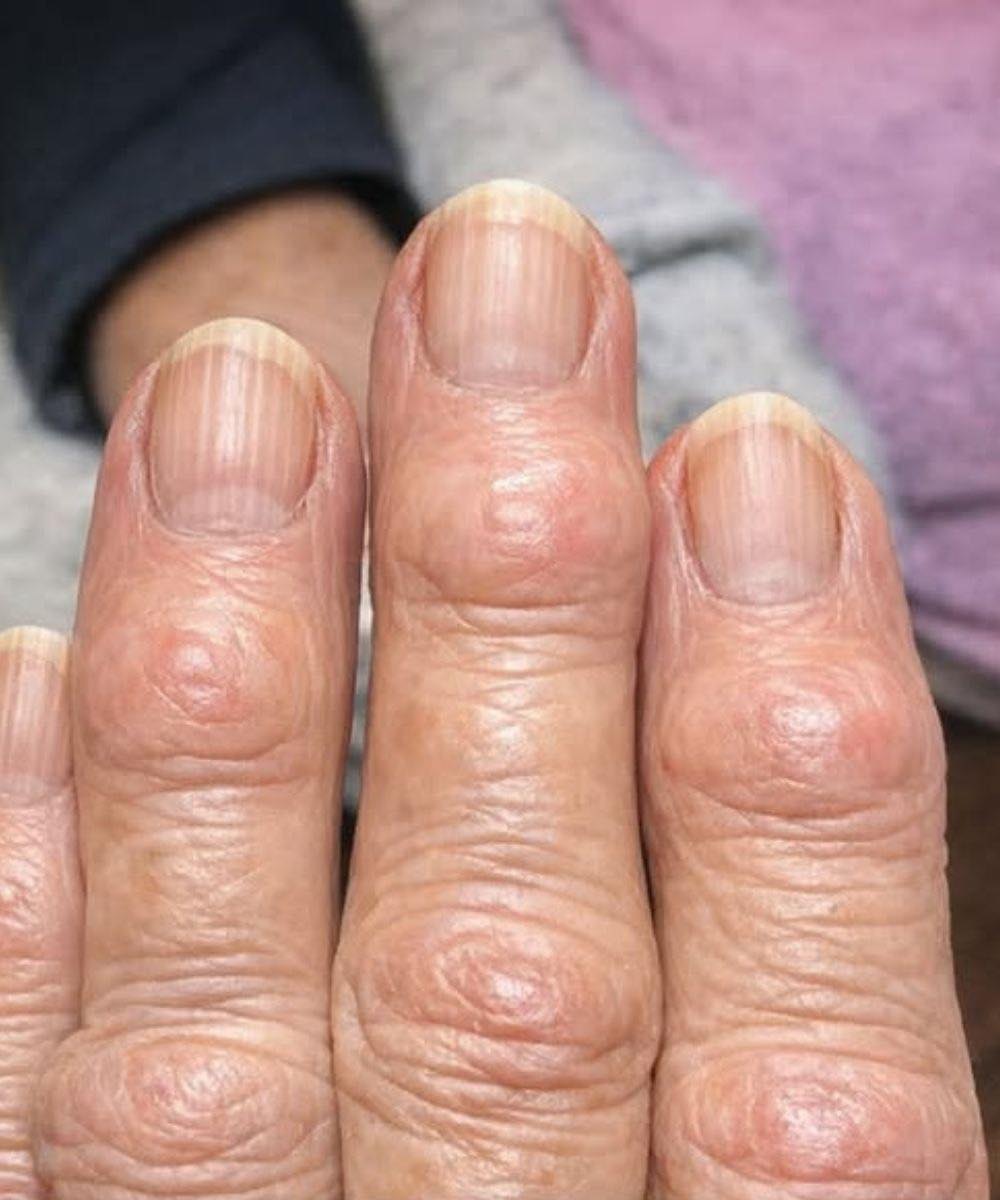
Hard bumps forming on finger joints near the nails in older adults are quite common, and while they can look concerning—especially if they seem to be spreading—they are usually linked to a specific joint condition rather than an infection or something “spreading” in the traditional sense.
The most likely cause is a form of osteoarthritis known as Heberden’s nodes. These are bony enlargements that develop at the joints closest to the fingernails (called the distal interphalangeal joints). They often appear gradually and may affect multiple fingers over time, which can give the impression that the condition is spreading from one finger to another.
Osteoarthritis itself is a degenerative joint disease. Over the years, the cartilage that cushions the ends of bones wears down. As this protective layer thins, the body tries to repair the damage by forming extra bone tissue. These small bony growths are what you see as hard bumps. Because this process can occur in multiple joints, especially in the hands, it’s not unusual for more bumps to appear over time.
Another similar condition involves bumps slightly lower on the fingers (at the middle joints), called Bouchard’s nodes. While your description points more toward the joints near the nails, it’s helpful to know that osteoarthritis can affect different parts of the fingers simultaneously or progressively.
You might wonder why this is happening now or why it seems to be getting worse. Age is the biggest factor. As people grow older, joint wear and tear accumulates. Genetics also play a role—if other family members have had similar hand changes, your grandma may be more prone to developing them. Repetitive use of the hands over many years, such as cooking, sewing, or manual work, can also contribute to joint stress and eventual changes.
The “spreading” you’re noticing is not contagious or infectious. Instead, it reflects the progression of osteoarthritis in different joints. One finger may develop a bump first, followed by others as the same degenerative process affects additional joints. This progression can be slow and may occur over months or years.
In the early stages, these bumps can be tender, swollen, or even slightly warm. Your grandma might have experienced pain or stiffness before the bumps became firm. Over time, the pain often decreases, and the bumps harden into permanent bony changes. Some people also notice reduced flexibility or slight deformity in the fingers.
There are a few other possibilities, though they are less common. For example, mucous cysts (fluid-filled sacs) can form near the nail and may look like bumps, but they are usually softer and sometimes translucent. Another condition, Rheumatoid arthritis, can affect the hands as well, but it typically involves different joints (closer to the hand rather than near the nails) and is often accompanied by significant swelling, warmth, and systemic symptoms like fatigue.
Although these bumps are generally harmless, they can affect hand function or cause discomfort. It’s a good idea to have a healthcare provider examine them to confirm the diagnosis and rule out other conditions. A doctor may recommend simple treatments such as anti-inflammatory medications, warm compresses, or hand exercises to maintain mobility. In some cases, topical creams or splints may help reduce discomfort.
Lifestyle adjustments can also make a difference. Gentle hand exercises can help maintain flexibility, while avoiding excessive strain on the joints may slow progression. Using ergonomic tools or assistive devices for daily tasks can reduce stress on the fingers.
If the bumps are painful, rapidly changing, or accompanied by redness or discharge, medical attention should be sought promptly, as these signs could indicate something other than typical osteoarthritis.
In summary, what you’re seeing is most likely a natural, age-related joint change rather than something dangerous or contagious. The appearance of new bumps over time reflects the gradual progression of joint wear rather than true spreading. While it can’t be completely reversed, proper care and medical guidance can help manage symptoms and maintain comfort and function in the hands.